Quick summary⚡
- What it is: In short, it’s extra pressure on the ulnar side of the wrist where the end of the ulna compresses the TFCC (a shock-absorber) and the lunate/triquetrum bones. 🧱➡️🧽
- How it feels: Typically, there’s an achy or sharp pain on the pinky side, which gets worse with pronation (palm down), ulnar deviation (bend toward pinky), and power grip (lifting, racquet swings, push-ups). Additionally, you may notice clicking. 🌀✊
- Why it happens: Sometimes the wrist is ulnar-positive (the ulna sits a bit longer); furthermore, prior fractures can shorten the radius, and certain sports or jobs load that side heavily. Importantly, pronation plus a clenched fist temporarily increases the load—so even “normal” X-rays can still coincide with real-life pain. 🧮
- Do most people need surgery? No. In fact, most improve with a targeted, stepwise, non-operative plan. Consequently, surgery is for the minority who still have clear mechanical pain after a proper trial. ✅
What’s actually going on? 🧠
Think of the TFCC as a pad + set of ligaments on the pinky side of your wrist. When the ulna pushes too much on that area—because of bone shape, past injury, or repetitive loading—the pad and nearby cartilage become irritated. That’s ulnar impaction. 🔧
However, here’s a key nuance: scans can show TFCC “tears” even in people with no pain. Therefore, we don’t treat images—we treat you. Moreover, straps/braces can help symptoms by limiting painful positions, not by “shortening the ulna.” (They don’t change bone length.) 🎯
Common symptoms 📋
- Pain or deep ache on the ulnar (pinky) side
- Worse with twisting, heavy gripping, push-ups, bat/club/racquet strokes, or weight-bearing on the hands
- Possible clicking or a feeling of “something catching”
- Reduced grip strength during flares
Red flags (seek urgent care) 🚑: traumatic deformity, fever/redness/heat, numbness/weakness into the hand, or inability to move after a significant fall. If any of these occur, please seek immediate assessment.
How we make the diagnosis 🔍
- History & hands-on tests that load the sore side in safe ways. Crucially, we compare painful and non-painful positions. 🖐️
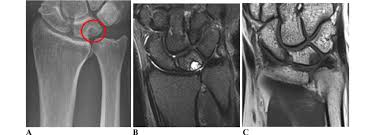
- Standardised X-rays (this matters):
- First, a neutral PA view (forearm neutral, no grip), and
- then a pronated clenched-fist view (to reveal the load that bothers you in real life). 🧪
- MRI (sometimes with dye) if we need to see the TFCC and cartilage; CT if we’re checking joint alignment. In many cases, this clarifies the picture. 🖼️
- We always interpret scans in the context of your symptoms, not the other way around. Consequently, your story leads the plan. 🧩
First-line treatment (most people get better here) 🛠️
Phase 1 — Settle it down (2–6 weeks) 🧘♂️
- Unload the hotspot: Start with a short period in a forearm-based brace or strap; additionally, avoid sustained pronation/ulnar deviation and heavy gripping.
- Pain relief: Use simple analgesics/NSAIDs if appropriate; alternatively, a cortisone injection can help calm a stubborn flare. 💉
- Everyday tweaks: Keep the wrist neutral for lifting, choose thicker handles, and avoid push-ups on flat palms (use dumbbells/handles). 🏋️♀️
Phase 2 — Restore motion & capacity 🔄
- Range of motion: Initially, move out of the most provocative angles; subsequently, re-introduce them gradually.
- Strength: Build forearm rotators (pronation/supination), improve ECU–FCU coordination, and progress grip endurance starting in neutral wrist positions.
- Technique coaching: Learn how to hold, push, pull, or swing without overloading the ulnar side. As a result, you’ll tolerate more activity with less pain. 🧑🏫
Phase 3 — Return to full sport/work 🚀
- Gradual re-exposure: First rebuild time-under-tension and volume; then, chase max power.
- Protection when needed: Use tape/brace for higher-risk sessions; meanwhile, plan recovery days. 📆
Many patients improve meaningfully in 6–12 weeks with this structured approach. ⏳✨
“Do I need surgery?” Usually, no—here’s when we consider it 🩺
We talk surgery only if mechanical, side-specific pain persists after a proper, targeted program. In other words, we earn surgery.
Two main procedures, explained simply:
- Arthroscopic wafer (key-hole trim): the surgeon gently trims a few millimetres from the very end of the ulna inside the joint to create space and reduce pressure. Pros: less invasive, faster recovery, and fewer complications for many. 🔧
- Ulnar shortening osteotomy (USO): a small section of ulna is removed in the shaft and the bone is plated to heal shorter. Pros: definitive shortening when the ulna is clearly long or wafer isn’t suitable. Trade-offs: longer healing and potential hardware irritation. 🧱➡️📏
Recovery ballparks:
- Wafer: expect light activity in ~2–4 weeks. 🗓️
- USO: anticipate immobilisation until bony union (~6–8 weeks), followed by progressive rehab (3–4+ months for heavy/manual sport). ⛑️
If your main problem is instability from a deep TFCC detachment, the solution may be TFCC repair (reattaching the ligament), not a bone procedure. 🧵
A balanced take: Some surgical improvement also comes from rest + protected loading + rehab that every post-op pathway enforces. Therefore, we choose the least-invasive operation that matches the real problem (space vs stability). 🤝
Self-care tips that actually help 💡
- Modify push-ups: Swap flat-palm push-ups for handles or incline while settling; consequently, you’ll reduce painful compression.
- Change your grip: Use thicker grips/over-grips on tools and racquets; as a result, you’ll stress the area less.
- Lift smarter: Keep the wrist near neutral for heavy lifts; likewise, avoid end-range bend toward the pinky.
- Progress slowly: Build forearm rotation strength gradually—quality reps > heroic loads.
- Plan recovery: Schedule recovery days the way you plan training days; consequently, your tissues adapt better. ✔️
FAQs 🙋♀️🙋♂️
Will my TFCC tear always cause pain?
No. TFCC changes are common in pain-free people, especially with age. Therefore, your story and exam matter more. 🧭
Does a WristWidget® “shorten the ulna”?
No. Braces can limit painful positions and improve tolerance; however, they don’t change bone length. 🔒
How long to calm down without surgery?
Most people notice clear progress by 6–12 weeks with the right plan. If you hit a setback, simply adjust load—don’t abandon the plan. 🛤️
If I need surgery, will it “fix it forever”?
Surgery can reduce the mechanical pressure or restore stability; nevertheless, long-term success still depends on good rehab and technique. 🔁
Want help in Melbourne? 📍
If you’d like a assessment and a clear, step-by-step plan, click here to book online. We’ll review your imaging, calm the flare, rebuild capacity, and only talk surgery if the mechanics truly demand it. 🙌
